Brain surgery is a medical subspecialty that deals with surgical disorders in the area of the brain.
Also, known as neurological surgery or neurosurgery.
It covers prevention, diagnosis, surgery and the rehabilitation process of neurological disorders.
All parts of the neurological system, including the part of the brain, spinal cord, nerves present all over the body and the blood vessels of this system fall under this domain.
The doctors who specialize in this field are called neurosurgeons. [1]
Neurosurgeons are trained to carry out these operations with great focus and care.
The following paragraphs aim to answer your general questions.
Table of Contents
How is a Brain Operation Done?
Like any other medical domain, neurosurgery is also ever-evolving.
New techniques and instruments are coming with every passing day that is allowing surgeons to perform procedures with great precision and better outcomes.
However, the basics remain almost the same.
There are different types of brain surgeries. Some are discussed below.
Craniotomy
A craniotomy can be carried out either by making a hole in the brain or by lifting a bone flap.
In closed surgeries, a hole is made in the skull and the brain is accessed. It is called a burr-hole craniotomy.
In open type surgeries, a part of the skull is removed and the surgery is performed. The removed part of the skull is then placed back and stitched. [2]
Endoscopic Surgery Via Nose
It is a type of minimally invasive surgery. In this procedure, a camera is introduced in the brain via the nose in order to visualize the part that needs surgery. The procedure is carried out without making any incision on the skull superficially. [3]
Endoscopic Surgery Via Skull
This type of surgery is also minimally invasive but it involves introducing a camera and instruments through small holes in the skull. [3]
Peripheral Nerve Surgery
In the case of peripheral nerves, the nerve is accessed by making skin incision in the area where the nerve is superficial and most easily accessible. It can be carried out to treat spinal issues as well.
Stereotactic radiosurgery (SRS)
This is a non-surgical procedure that is most commonly used to treat functional abnormalities and other types of small tumors in the brain by delivering targeted radiation. Therefore it requires less high-dose treatments which will hopefully help in the preservation of healthy tissue
What do You Need Surgery For?
There is a multitude of health issues that may require surgery in the area of the brain. These indications can range from an infection to a dangerous tumor.
They are discussed below. [4]
Stroke
Stroke is one of the common indications of requiring surgery. The incidence of stroke or brain hemorrhage is high in the present times due to various underlying risk factors.
When a stroke happens, the blood can accumulate in the affected brain region.
This blood applies pressure on the surrounding structures causing brain dysfunction. In such cases, there is a need to remove the accumulated blood, and surgery is carried out.
Brain Tumor
Different benign and cancerous masses can grow in the brain and other neurological structures. They compress the surrounding structures and cause bothersome symptoms like headaches, body weakness, etc. To treat this situation, the tumor is removed via surgical procedures.
Brain Aneurysm
When a blood vessel balloons up in the brain, it is called an aneurysm. This blood vessel can rupture easily leading to life-threatening complications. Procedures are carried out to get rid of aneurysms.
Hydrocephalus
Cerebrospinal fluid (CSF) is a fluid present around the brain that protects and nourishes it. In some cases, the amount of this fluid can become more than normal. This leads to various symptoms and hence, it needs to be treated. The fluid is drained via surgery.
Trauma
Trauma caused by any kind of mechanical injury can cause bleeding and brain damage. Emergency surgery is often required to repair the damaged brain.
Brain Abscess
A brain abscess can form following a brain infection. Sometimes, antibiotics alone do not work.
Draining abscess becomes vital because it keeps damaging surrounding structures otherwise. The drainage process is carried out via neurosurgery.
Epilepsy
Sometimes, the cause of epilepsy, fits or convulsions is mechanical. There can be some physical abnormality leading to these problems. In such cases, surgery is done for definite treatment.
Parkinson's Disease
A surgical procedure known as deep brain stimulation (DBS) is most frequently performed as a treatment for Parkinson’s.
A surgeon will place thin metal wires in the brain which then send electrical pulses in order to help the brain gain some control of some of the associated motor symptoms.
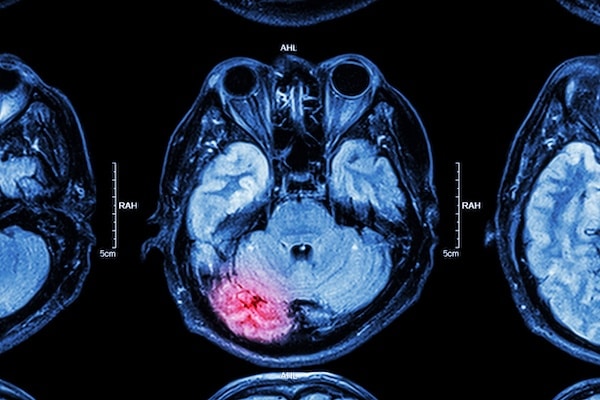
What is the Most Common Brain Surgery?
The most common is called a craniotomy. This surgery is carried out under general anesthesia that means the patient is put to sleep. Skull base and brain layers are incised to reach the brain tissue.
The incision is carefully made over the area that requires treatment.
A pre-requisite for this surgery is multiple brain scans that allow the surgeon to visualize the pathology clearly and plan surgery accordingly.
The surgeon also refers to these scans during the procedure to avoid mistakes and increase precision. These scans are also fed to the computer that guides during this procedure.
Various instruments are used to carry out the procedure. Once the process is complete, the brain layers are stitched back and the removed or incised part of the skull is then placed back with the help of metal stitches and lastly, the skin is stitched.
In some cases, awake craniotomy (awake brain surgery) is also performed. It is usually done in cases where the surgeon needs to ask you to perform a few functions in order to check if surgery is going right.
The patient might be asked to speak or move a part of the body. The patient might be awake for the whole time or for a small time during the surgery.
A craniotomy is done for various purposes, such as after a stroke and to remove a tumor. [5]
How Many Hours is Brain Surgery?
The duration can differ. Some surgeries are simple and easy and require a small-time, while others are long and complex and require many hours.
The estimated duration is mentioned below.
- A craniotomy takes 3 to 5 hours.
- An awake craniotomy takes 5 to seven hours.
- A biopsy procedure can take 1 to 2 hours. [6]
So, the time window usually varies between one hour to up to seven hours or even more.
It usually depends on the complexity of the disease and the expertise of the surgeon.
An experienced surgeon can perform the same surgery in much lesser time as compared to a trainee or junior doctor.
What are the Chances of Surviving Brain Surgery?
Neurosurgery is a rapidly developing field with new research studies pouring in every day.
These studies and findings are helping improve diagnosis, treatment, and prognosis in the field of neurosurgery it is always considered a risky surgery, and it scares most patients.
However, with the recent advancements and techniques, brain surgeries have a much better outcome than before.
The mortality rate used to be higher in the past. However, the success rate has increased giving patients a fair chance of survival and normal life.
In a study conducted on patients with brain, metastasis showed that the survival rate was much higher than expected. 73.23% of patients showed improvement after the surgery to remove brain metastasis. 55% of patients had a survival of more than six months. [7]
The important thing to consider here is that after a metastatic brain disease, survival rates are very low without treatment. So, carrying out surgery definitely enhances the life span of terminally ill patients as compared to those who do not undergo any intervention.
Another study analyzed the survival rate after a stroke attack.
About 80% of patients die after a brain hemorrhage if treated with medication rather than surgery. Performing surgery to remove the blood in order to decompress the brain significantly improves the survival rate.
There is always some risk of disability but patients live a longer life as compared to the ones who do not undergo surgery. [8]
How Long Does it Take to Recover From Brain Surgery?
It may take a different amount of time to recover from surgery on a per-patient basis. There are many factors that can contribute to early or late healing.
These factors vary among different people. The following are a few factors that can delay recovery.
- Old people take a longer time to cover.
- People with a weaker immune system require more time.
- Wound infection prolongs healing.
- People take more time to recover after a complex surgery.
- Malnourishment delays recovery time.
- The strain on the wound can be a factor.
- Cough has a negative impact on wound healing.
Now let’s look into the factors that are associated with faster healing.
- Younger patients heal faster.
- A strong immunity has an important role.
- Taking antibiotics and other medications as prescribed helps with recovery.
- Proper wound cleaning and care have an essential role.
- Regular follow-ups with your doctor are necessary.
Usually, you are supposed to stay at the hospital for up to 10 days after surgery.
The time may increase depending on the condition of the patient. The skin takes a few days to a few weeks to heal. It may take up to 2 months to recover after surgery.
Rehabilitation services are provided after surgery that helps aid faster recovery. A physiotherapist helps in restoring movements.
The patient may also need speech and occupational therapists in order to help with different body functions. [9]
How Dangerous is Brain Surgery?
Again, there is no definite answer to this question. The prognosis of brain surgery differs from person to person.
A neurosurgeon weighs benefits of performing an operation against its drawbacks, and the surgery is only carried out if its benefits are more than the problems associated with it.
Also, the outcome of surgery is kept in mind. Patients who have multiple comorbidities and are not suitable for surgery because of high mortality are not considered.
There are many complications that can be faced. The most important ones are listed below.
- A patient may have severe pain after the surgery. Strong painkillers are used to treat it.
- There can be irritability.
- A patient can be drowsy or unconscious.
- Massive bleeding can occur.
- There are chances of wound infection.
- A patient can have seizures.
- There is a risk of stroke.
- The brain can swell up.
- There can be speech problems.
- A patient can experience weakness in any part of the body.
- There can be vision and coordination problems.
- There can be hearing problems.
Neurosurgeons are ready to tackle these situations. All the possible complications are communicated to the patient and his or her family before the procedure.
Medications are prescribed to avoid problems like bleeding, infection, pain and brain inflammation.
Other problems like body weakness, speech problems, and balance problems can be faced for a short time, and they usually go away on their own.
However, in some cases, there is a risk of permanent disability. [9]
Can You Die from Brain Surgery?
The worst complication of surgery can be death. There can be various risk factors that can increase the risk of mortality.
A study was conducted on patients who underwent craniotomy.
The results showed that the mortality rate was 2.3% within the first month of the surgery, and the most important risk factor associated with a high mortality rate was old age.
Patients older than 60 years had a higher chance of death. [10] Another study observed the rate of death after surgery among brain tumor patients.
Out of all surgeries included in the study, 72% of surgeries were performed on the brain. The mortality rate in the first 30 days after was 3%.
The study was conducted again after doubling the number of surgeons for these surgeries and the mortality rate dropped by 20%. [11] This shows that increasing the number of surgeons can improve the outcome.
The recent advances in the field of neurosurgery have definitely improved the outcome of brain surgeries.
Like any other surgery, there are still some chances of complications like death that depend on so many factors.
However, surgery is now safer than ever before and has many positive implications as compared to conservative treatment.
You Can View Other Sections Of Brain-Surgery.com Below
- Stroke – What Are The Symptoms?
- Aneurysm Surgery
- Arteriovenous Malformations
- Cavernous Hemangiomas
- Intracerebral Hemorrhage
- Subdural Hematomas
- Children's Brain Tumors
- Benign Brain Tumors – A Further Look At Potential Diagnosis
- Acoustic Neuromas
- Astrocytoma
- Meningioma
- Pineal Tumors
- Pituitary Tumors
- Ependymoma
- Glioblastoma Multiforme (GBM)
- Malignant Astrocytoma
References
- https://en.wikipedia.org/wiki/Neurosurgery
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2640049/
- https://www.ncbi.nlm.nih.gov/pubmed/15527092
- https://www.ncbi.nlm.nih.gov/pubmed/10093670
- https://www.ncbi.nlm.nih.gov/books/NBK482297/
- https://www.pennmedicine.org/for-patients-and-visitors/find-a-program-or-service/neurosurgery/brain-tumor-center/brain-tumor-surgery-faq
- https://www.ncbi.nlm.nih.gov/pubmed/27667577
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6333741/
- https://www.cancerresearchuk.org/about-cancer/brain-tumours/treatment/surgery/recovering
- https://www.ncbi.nlm.nih.gov/pubmed/21273920
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5129829/
